"Overview from HYTM 10k
Traditional treatment approaches for substance dependence focus mainly on group therapy, abstinence, and behavioral modification, while the disease’s underlying physiology and pathology is rarely addressed, resulting in fairly high relapse rates. Currently therapies are beginning to target brain receptors thought to play a central role in the disease process. We believe that our PROMETA protocols offer an improvement to traditional treatments because treatments with PROMETA are designed to directly target the pathophysiology induced by chronic use of alcohol or other drugs. Without specific treatment, the abnormalities in brain function induced by chronic drug dependence may take months to years of drug abstinence to return to normal function. We believe the PROMETA protocols offer an advantage to traditional alternatives because they provide a treatment methodology that is discreet, mildly sedating and that can be initiated in only two to three days, with a second two‑day treatment three weeks later for addictive stimulants. Our PROMETA protocols also provide for one‑month of prescription medication and nutritional supplements, combined with psychosocial or other recovery‑oriented therapy chosen by the patient in conjunction with their treatment provider. Initial clinical observations suggest that our protocols may improve cognitive function, reduce withdrawal symptoms, be associated with higher initial completion rates than conventional treatments, and reduce physical cravings which can be a major factor in relapse, thus allowing patients to more meaningfully engage in counseling or other forms of psychosocial therapy. These conclusions were reached during treatment of approximately 400 patients and may not be confirmed by clinical research studies, may not be statistically significant, have not been subjected to close scientific scrutiny, and may not be indicative of the long‑term future performance of our protocols.
We believe the short initial treatment period when using our PROMETA protocols is a major advantage over traditional inpatient treatments and residential treatment programs, which typically consist of approximately 21 days of combined inpatient detoxification and recovery in a rehabilitation or residential treatment center. Treatment with PROMETA does not require an extensive stay at an inpatient facility. Rather, the protocols offer the convenience of a two to three day treatment (addictive stimulants require a second two day treatment three weeks later) and can generally be administered on an outpatient basis. This is particularly relevant since approximately 77% of adults classified with dependence or abuse are employed, and loss of time from work can be a major deterrent for seeking treatment. Moreover, we believe PROMETA can be used at various stages of recovery, including initiation of abstinence and during early recovery, and can complement other forms of alcohol and drug abuse treatments. As such, our protocols offer a potentially valuable alternative or addition to traditional behavioral or pharmotherapy treatments that does not require chronic administration of a pharmacotherapy, thus minimizing compliance issues. Many medications marketed to treat alcohol or drug dependence are not administered until the patient is already abstinent, require long‑term chronic administration and must be taken several times a day to achieve the desired effect.
Substance dependence is a worldwide problem with prevalence rates continuing to rise despite the efforts by national and local health authorities to curtail its growth. Substance dependence disorders affect many people and have wide‑ranging social consequences. In 2004, an estimated 22.5 million Americans suffered from alcohol or other forms of drug abuse or dependence, according to the National Survey on Drug Use and Health published by the Substance Abuse and Mental Health Services Administration (SAMHSA), an agency of the U.S. Department of Health and Human Services. Furthermore, according to the survey, approximately 12 million Americans age 12 and older, or 5 percent of the population, are reported as having tried methamphetamine, and the percentage of methamphetamine use characterized as abuse or dependence doubled from 2002 to 2004. Findings from The Drug and Alcohol Services Information System (DASIS) Report published by SAMHSA’s Office of Applied Studies in September 2004 show that methamphetamine hospital admissions as a percent of substance abuse treatment admissions increased from 1% in 1992 to 7% in 2002.
It is commonly reported that addiction to methamphetamine is an epidemic rapidly spreading throughout the U.S. Methamphetamine addicts are highly resistant to treatment and, even after intervention, relapse at very high rates. Methamphetamine use is also spreading to the workplace. A study funded by the Wal‑Mart Foundation in 2004 determined that each methamphetamine‑using employee costs his or her employer $47,500 per year in terms of lost productivity, absenteeism, higher healthcare costs and higher workers’ compensation costs. For county governments and their taxpayers, methamphetamine abuse causes legal, medical, environmental and social problems. A study entitled “The Criminal Effect of Meth on Communities” conducted in 2005 by the National Association of Counties, which surveyed 500 counties in 45 states, reported that 58% of counties surveyed reported methamphetamine as their largest drug problem, with 87% reporting increases in arrests involving methamphetamine starting 3 years ago. Cocaine was reported as the number one drug problem in 19% of the counties. There are currently no generally accepted medical treatments for cocaine or methamphetamine dependence.
Summarizing data from the Office of National Drug Control Policy (ONDCP) and the National Institute on Alcohol Abuse and Alcoholism (NIAAA), the economic cost of alcohol and drug abuse exceeds $345 billion annually in the U.S., including $41 billion in healthcare costs and approximately $245 billion in productivity losses. Despite these staggering figures, it is a testament to the unmet need in the market that only 17% of those who need treatment actually receive help. Traditional treatment methods are often not particularly effective, especially when it comes to those who are dependent on stimulants. Often faith, willpower, and counseling are the only options available. Compounding the lack of efficacious treatment options is the enormous stigma of leaving one’s life, income, and loved ones for weeks at a time to seek inpatient treatment.
There are approximately 13,000 facilities reporting to SAMHSA that provide substance abuse treatment on an inpatient or outpatient basis. Historically, the disease of substance dependence has been treated primarily through behavioral intervention, with fairly high relapse rates. The DASIS report states that in 2000 only 54% of those treated for alcoholism and 51% of those treated for cocaine and other stimulants complete detoxification, and that combined alcohol and cocaine outpatient treatment completion rates were only 41%. For patients who do complete treatment, the NIAAA reports relapse rates three months following treatment for alcohol dependence to be 50%. Relapse rates are higher for those suffering from cocaine dependence as opposed to alcohol. For the behavioral treatment of cocaine dependence, the Drug Abuse Treatment Outcome Survey reports a relapse rate of 69% one year
Our Solution: PROMETAÔ
Those suffering from alcohol and/or drug dependence have often been characterized as having social disorders or a lack of self‑discipline and, as noted above, there are relatively high relapse rates utilizing conventional treatment methods. While we believe the psychological approach to substance dependence treatment is important, we recognize that physiological factors of substance dependence should be addressed first to provide patients with an improved chance for recovery. We believe our physiological approach, focused on addressing the neurochemical imbalances in the brain caused or worsened by substance dependence, provides a substantial commercial opportunity.
Current research indicates that substance dependence is associated with altered cortical activity and changes in neurotransmitter function, which are critical to brain function. Moreover, changes in the neurochemistry of the brain underlie the hallmarks of substance dependence, including tolerance, withdrawal symptoms, craving, decrease in cognitive function and relapse. Our PROMETA protocols include medically supervised treatments, prescription medications and nutritional supplements, combined with psychosocial or other recovery‑oriented therapy chosen by the patient in conjunction with their treatment provider.
The PROMETA treatment protocols provide for:
· A comprehensive physical exam, including specific laboratory tests, prior to initiation of treatment by the treating physician, to determine if the patient is appropriate for the PROMETA protocol
· Medically supervised administration of prescription medications and nutritional supplements
· One‑month of prescription medications and nutritional supplements following the initial treatment
· Individualized continuing care options
Treatment with PROMETA involves the oral and intravenous administration of pharmaceuticals in a medically supervised setting. The medications used in the PROMETA treatment protocols have been approved by the FDA for uses other than treatment of substance dependence. The PROMETA treatment is discreet and does not require long periods away from home or work. Treatment takes place at a hospital facility, clinic or properly equipped outpatient setting by healthcare providers who have licensed the rights to use our PROMETA protocols. The treatment begins with a two‑to‑three day course of prescription medications and nutritional supplements. The PROMETA protocol for stimulant dependence provides for a second, two‑day course of treatment at the facility, which takes place about three weeks after the initial treatment .Some patients may require an additional day of treatment, subject to the treating physician making this decision during the course of the treatment. In general, the intravenous treatment session typically lasts about an hour. Some patients may receive their treatment in a hospital, or “in‑patient” setting. For these patients, the balance of time spent at the treatment facility or hospital is intended to ensure that the patient is well‑rested and comfortable between the relatively short treatment periods. Most patients take meals and choose to sleep much of the time between treatments. For the patients receiving care in an “outpatient” facility, such as a physician’s office or treatment center, their doctor may monitor them for a few hours following the treatment session. Typically, the patient would then be released to an accompanying person and return the following day for completion of their treatment. Following the medically supervised treatments, our protocols provide that patients receive one month of prescription medication and nutritional supplements, and participation in psychosocial or other recovery‑oriented therapy they select with their physician.
Analysis
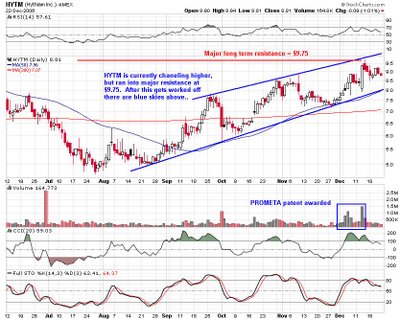
At first glance HYTM appears to be to good to be true. A simple 2-3 day treatment using off patent drugs eliminates the physical cravings of drug abusers. However, the inital studies have produced remarkable anecdotal evidence that PROMETA seems to really work. There are several double blind placebo controlled studies underway that should be completed in 2007. HYTM is charging a lot of money per treatment but the economic cost of drug abuse is staggering. HYTM needs to be on your radar screen because the upside potential plus media attention could be huge. The chart says the market is starting to believe.....
"
To follow up on Namec's comments, HYTM is in a space that has massive potential with few competitors. With a current market cap of only $350 Million next to a $40 Billion market the grow prospects are obvious. The two and a half year weekly chart above shows HYTM is about ready to breakout of a long period of consolidation. After moving up from the 2$ area HYTM has been rangebound for about two years between $5 and $9.75. On each push up towards resistance the volume has increased and the action has been more well behaved. What i mean by well behaved is how the stock reacts with respect to the moving averages. Specifically, on this last run HYTM held it's 50 dma more consistently than before. Also, the on balance volume has steadily been increasing while the stock has remained rangebound, that tells me the stock is being accumulated. I wouldn't jump into HYTM just yet, but as Namec said keep it on your watch list and watch for a move above key resistance at $9.75. If I see this thing trading at $10 or higher I will be all over a calendar spread on the $10 calls, and yes it trades options. However, if you really like the story you might try picking up shares at the 50 dma, or support at $7.50 if it pulls back that far. Happy holidays from us here at stock geometry!


No comments:
Post a Comment